Following are excerpts from the Partial Birth Abortion Ban trial in Nebraska.
Leroy Carhart, M.D., et. al. v. Ashcroft
U.S. District Court, District of Nebraska
The Honorable Richard G. Kopf, Judge.
Note: All pictures are of unborn babies who would be candidates for this type of abortion, which is usually performed in the late second trimester, but can be performed in the third.
Excerpts from direct examination of Dr. William Fitzhugh:
Q. All right. Going back now, I think you said in some instances when you use a suction cannula, that part of the fetus or the umbilical cord will come out through the cervix. Then what do you do at that point?
A. Well, if the umbilical cord comes down, I unattach that from its integrity. I just break it and pull on it. If a foot comes down, I grab the foot and pull down on that.
Q. If no part comes down, as a result of the suction, what do you do?
A. Then I have to place the ring forceps up into the uterus and find a part.
Q. And is there a particular part that you’re trying to grasp, at that point?
A. I take whatever I can get, because I have really — I have a feel of when you feel the cranium of the head, but that’s about the only thing I have a feel of when you grasp until you pull it down. I just pull down with the forceps and, you know, see what part you have, and see if you can get more of that part out. If you get more of the part out, you twist to try to get more tissue out. If that doesn’t happen, then you pull hard enough that it will disarticulate at that point or break off at that point.

Q. Do you have other concerns, when you find yourself in that situation, to cause you to use forceps to compress the skull?
A. As I mentioned earlier, my preference is that when I use a suction, my preference is that I obtain the umbilical cord and separate the umbilical cord. The one thing that I want–and I don’t want the staff to have to deal with is to have a fetus that you remove and have some viability to it, some movement of limbs, because it’s always a difficult situation.
Q. Can you tell the Court how often the fetus comes through entirely intact, without you having to do anything more to remove it?
A. It happens about two to five times a year. And in those situations, it will occur one of two ways. One is that the ladies has had some labor up to that point. And when I remove the speculum, the laminaria and sponges from the vagina, she’ll already have a foot in the vagina or two feet in the vagina. That’s one of the times it happens. And the other time it happens is when I reach up and deliberately grasp for something. I will get a foot, bring it down, and the whole body will come down. And it happens about two to five times a year.
Q. And in that situation, is the entire fetus coming out or is it any part of it remaining in the uterus? Is the head —
A. It can happen either way. I would say one time out of those that I will pull and everything will come out. I’ll pull and twist and everything will come out. And probably two or three times, I’ll have to pull and the head will get stuck against the cervix. So I’ll have to use my ring forceps and crush the skull.
~
Q. So other than drugs or making incisions in the cervix, could you simply detach the head at that point?
A. I guess you could, but then you would have to find it.

….
Q. Does it every happen that you would disarticulate a piece of the fetus, and then on the next pass, bring out the remainder of the fetus, except for the head?
A. Its happened that way, disarticulated up to a knee joint. You grab the next grasp and you brought most everything out.
Excerpts from the Government’s cross-examination of Dr. Fitzhugh:
Q. So when you’re doing the D & E procedure that you do, you expect dismemberment to occur; is that correct?
A. It happens in the majority of cases, not expected, but it sure would be nice if it happened more often.

Q. So one of the reasons that you use the forceps is to compress the skull is to ensure that the fetus is dead when you remove it?
A. That’s one of the reasons.
~
Q…..what actions do you take during a D & E that would be fatal to the fetus?
A. Well, number one, I like to interrupt the umbilical cord. Number two, we are working on a young gestation, but that’s not to do it. And we break up parts in the uterus and we crush skulls.
Q. When there have been instances where the — you have been doing a D & E and the fetus has come out intact, have you been aware of reactions from others in the operating room?
[Here counsel for the plaintiffs entered an objection, which the Court overruled.]
A. Yes, they certainly show more interest in that when it happens than they do on a routine situation.
Q. In fact, they gasp, don’t they, when that kind of thing happens?
A. Some of them gasp, yes, sir.
Q. Your impression in those situations is that they were probably having a harder time dealing with that situation; is that correct?
A. Yes, sir.
Excerpts from direct examination of Dr. Jill Vibhakar:
Q. And have you had any situations where the fetus is not necessarily coming out feet first but where part of the fetal trunk past the naval has come outside the mother?
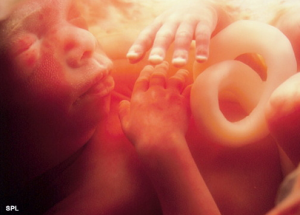
A. Yes, . . . the upper extremity is removed included [sic] the shoulder area, and sometimes when–sometimes when we are doing the D & E, some of the first things that are removed are maybe a portion of skin from the trunk or even ribs or other trunk contents.
Picture: Sometimes the shoulder or arm is removed first when aborting a baby this age, sometimes skin from the trunk or a rib
Q. And can the fetus still be living in that it has a heartbeat or other signs of life at that time?
A. Possibly, yes.
Q. Do you know when the removal of the fetus, fetal demise occurs?
A. No, I don’t.
Q. Is there any clinical significance to when you cause fetal demise during the procedure?
A. Not in my opinion.
Excerpts from Government’s cross examination of Dr. Vibhakar:
Q. Okay. When the head was struck, you disarticulated [detached] the body from the head; is that correct?
A. Yes.
Q. And you removed the body, compressed the head and removed the head; is that correct?
A. Yes.
Q. And in decompressing the skull, you’re trying to reduce its sides [sic] so it can fit through the cervix?
A. Yes.

Q. And when you are doing this, you’re trying to remove skull pieces so the liquid brain will empty from the cranium and the head will decrease in size; is that correct?
A. And in compressing it, if it doesn’t fit, and in my experience it hasn’t fit without decompressing it in the process of crushing it or grasping it, it becomes punctured enough so that the cranial contents will drain, and then it will fit through the cervix.
Excerpts from Abortion Doctors’ direct examination of Dr. William Knorr:
Q. Can you tell the Court approximately how many abortions you performed last year?
A. Somewhere between five and six thousand.
Q. Of those, can you estimate how many were second trimester abortions?
A. Somewhere between 12 and 15%.
….
Q. Dr. Knorr, before you begin to remove the fetus during a D & E procedure, is the fetus typically alive?
A. . . . . the majority of the fetuses are alive.
Q. And you don’t routinely induce fetal demise, as part of your second trimester abortion procedures, is that right?
A. That’s right. Very rarely.
Q. And why not?
A. I just don’t believe in it . I think that it’s an extra procedure and, you know, we first have to remember, don’t do any harm.

Q. When it happens and the fetus comes through the cervix except for the head, how do you proceed?
A. I first evaluate the cervix to see if I have enough room to slip a finger between the cervix and the fetal head, and if I can do that, I can then insert my crushing forcep around the head, crush the head and extract it. If the cervix if very tight, I can’t do that, I will use a craniotomy procedure, will turn the fetus so the back is up and find the area that I want to open, and either with a finger, dialator or a scissor will open that area and gently pull down. That pressure alone is enough to empty the cranium and extract the head.
Excerpts from Government’s cross examination of Dr. Knorr:
Q. Also when you bring out a fetus in pieces, you make sure that you have got all the parts that you want; right? You kind of —
A. Yes.
Q. You try and lay them out and put them back together as best you can to see if you have everything?
A. Not necessarily. Some of us keep track on the way out.
Excerpts from direct examination of Dr. Leroy Carhart, M.D.:
Q. Okay. And, Doctor, is the fetus living at the point at which it’s stuck at the calvarium [head], lodged at the cervical os?
A. Normally, my 16 and 17-week patients are — the fetuses are alive at the time of the final delivery.
Q. And what’s your next step, at that point, if the fetus has lodged at the cervical os?
A. Under 17 weeks, I would use a forcep. …remove the part of [the] fetus that was easily reachable. Hopefully try to use small bites to work the way up and remove the rest of the fetus so that it comes out intact. If not, then remove whatever part that I could get easily and then go back and remove the rest.

Q. Okay, Doctor, have you had a circumstance…where the fetus has been not intact, partially dismembered, and yet part of the fetal trunk passed the naval passed the umbilicus, has come outside the body of the mother?
A. ….But, certainly, when an upper extremity comes through the vagina, and I have to remove it, at that point — the shoulder, the shoulder joint actually tends to be more substantial than other joints in the body. So mostly if I can grab above the elbow, I will get part of the scapula, and sometimes even part of the chest wall from that extremity; ribs, and possibly even lung tissue or other tissue inside of the chest cavity.
Q. Doctor, focusing on your 12 through 17-week procedures, can you tell me, does the cervical dilation that you achieve have any effect on the size of the fetal parts that you’re able to remove?

A. Yes, ma’am. I can normally remove, virtually intact, as I said, two, three pieces. I can often get up to the base of the skull then go back and remove the skull. I can often get both lower extremities, and divide somewhere at the upper part of the spinal cord, removing abdominal organs and some even thoracic organs on the very first removal.
Excerpts from cross examination of Dr. Carhart:
Q. Do you agree with the statement, Doctor, that dismemberment at 20 weeks and beyond is difficult due to the toughness of the tissue at that stage of the development?
A. I think it’s fair to say that, yes, sir.
Q. And would you agree that it’s fair to say that because of the progress and the ossification and calcification of the fetal bones as gestation increases, it becomes more difficult to dismember the fetus after 19 weeks?
A. ….I don’t think that up through 24 weeks anybody would say that it’s truly a difficult procedure. It’s more difficult as the gestation increases.
….
Q. So would you agree, Doctor, that in the process of disarticulating [removing] a fetal part is a process of traction, counter-traction, grasping what you can get ahold of, pulling it down through the cervical os and rotating to dismember the part; is that a fair statement? A. If one is trying to disarticulate, yes.
….
Q. In those instances then, where the head is stuck in the os you testified a moment ago you’ll either compress or open the skull to drain, correct? A. Yes, sir, if traction alone, yeah, compressing, grabbing and bringing it down that alone doesn’t work, yes, sir.
Q. You try the compression and grabbing first?
A. I usually try to remove it manually before I use any instruments, yes, sir.
Q. And what informs your decision on whether either to open the skull and have the fetus drained or have the head drained or use forceps or some other means of compressing the skull?
A. Well, I don’t know if I can put that into words. It’s a judgment call at the time.

…..
Q. Your declaration says you use a sharp instrument to open the skull on those occasions on which you do it?
A. I have to see that. I don’t even own a sharp instrument in my clinic.
Q. Yeah, 22, last, second-to-last sentence [referring to Carhart’s earlier declaration], I use a sharp object either under direct visualization or with real-time ultrasonography to penetrate or enter the fetal skull.
A. Well, my actual choice is a uterine packing forceps, but I would accept that that could be, by some, considered sharp. I’m not saying there is anything wrong with this.
Q. You consider that forceps to be more of a blunt instrument; is that correct, Doctor?
A. I generally like to open the tissue slowly and dissect it apart the same way much like you’re doing surgery because you’re less likely to involve any other structures, and if you do, you’re not causing a vast amount of problems. It’s rather limited.
….
Q. My question is, simply, I want to get to the actual process that you utilize in trying to bring the fetus out intact.
A. I rarely try to dismember a fetus after the 20th week. I’m not sure I understand how to get my point and what I’m doing to be understood. If I — if nothing is coming through the os and nothing has come through the os and it appears to be that waiting another hour or four hours is going to not produce any different change than what I have seen already, at that point we will put the patient in the operating room and remove the fetus. I may grab a foot and bring it down. …If I bring an arm down and bring it outside of the uterus and possibly even outside of the vagina, depending on where the uterus is, I’m not going to put that arm back inside of the woman’s body to take that bacteria back inside, so I’ll remove that arm….
…..
Q. You recommend the use of ultrasound?
A. If — I think for second trimester D & E, it would be considered not within the standard of care to not have obtained an ultrasound. I don’t think there is a standard of care that involves the real-time, as you’re doing it, ultrasound. I know many, many doctors do not do that, [and] they do very well. I also know that I sleep better at night when I know what I’ve done.

…..
Q. Do you know how common it is for a pregnancy to be terminated for a maternal physical health reason?
A. Not in the United States. In my practice in Omaha or in Nebraska, my practice. It’s fairly rare.
THE COURT: Okay. Now, once again, in the ages that we are talking about here, the later ages, 18 weeks to 24 weeks, are there any circumstances where you in the recent past have been unable to cause fetal demise by use of injection?
WITNESS: Yes, sir, there was one incident where that happened with a 21 week twin pregnancy, and can I describe – – ….She was a multi-parous patient, and I attempted with her to do the fetal injection first which used to be my practice. I thought I had obtained adequate, that I had obtained that, and I started to place laminaria and very shortly. By the time I had put in the third or fourth laminaria, I started to get bleeding, and it just became worse and worse as time went on. …we gave her everything to try to constrict the uterus because if you can impact the fetus into the uterus, you can cause enough construction to slow the blood flow down. . ..However, one of the twins had, I thought, probably was dead. The other one, I’m sure, was not, but I had to remove both of those fetuses in virtually a nibble-nibble fashion. I don’t know how else to describe it, because I had an opening, the maximum I could get was like maybe one-anda-half to two centimeters which was not adequate to deliver the fetuses.
Excerpts from redirect examination of Dr. Carhart:
Q. ….The procedure you talk about from 14 to 17 weeks where you were able to remove the fetus intact or largely intact up to the calvarium, if the next step was the compression or collapsing of the skull, whichever method you use to do that, could that cause fetal demise?

A. I think it eventually would. It may not cause immediate fetal death though. I mean, the fetus is going to die.
Excerpts from re-direct examination of Dr. Watson Bowes, Jr.: Q. And, Doctor, what is your opinion concerning the medical necessity of partial-birth abortion procedures such as intact D&E with regard to preserving the health of the mother?
A. Well, I will restate what the American College of Obstetricians and Gynecologists said in their statement. They know of no instance where it’s necessary to use this procedure to — they could think of no specific instance when this procedure would be necessary to protect the health of the mother.
Excerpts from direct examination of Dr. Kanwaljeet Anand:
Q. So, Doctor, do you have an opinion as to whether the partial-birth abortion procedure causes pain to the fetus?
A. If the fetus is beyond 20 weeks of gestation, I would assume that there will be pain caused to the fetus. And I believe it will be severe and excruciating pain caused to the fetus.
Q. What do you mean by severe and excruciating pain?
A. You see, the threshold for pain is very low. The fetus is very likely extremely sensitive to pain during the gestation of 20 to 30 weeks. And so the procedures associated with the partial-birth abortion that I just described would be likely to cause severe pain, right from the time the fetus is being manipulated and being handled to the time that the incision is made, and the brain or the contents, intracranial contents, are sucked out.
Excerpts from direct examination of Dr. Leroy Sprang:
Q. Okay. Doctor, if I could, I wanted to ask you, based on your training, experience as an OB/GYN, your knowledge of medical literature, do you have an opinion as to whether the intact D & X procedure presents significant risk to the woman?
A. I believe it does.
Q. Could you just briefly list kind of what those risks are?
A. My concerns with the procedure are several things that distinguish it from the traditional D &E. The fact that it — more commonly for D & E, you can dilate the cervix over one day. There may be exceptions. But in general, more commonly one day. More commonly for a D & X, you’re dilating it over two days.
Q. Does that present a risk?
A. Presents several problems. Laminaria are these little seaweed sticks that you’re placing in the uterus, and they have to cover the entire length of the cervix. They have to be from the outside to the inside to make sure the entire cervix dilates evenly. Again, infectious disease is my area of expertise. Bacteria have a better chance moving along the laminaria and getting inside the endocervical os and running a risk of infection, because they are in contact with the vagina, and up against the amniotic sack. That’s the issue.
…..
A: In the descriptions I have read on occasion, including Haskell, he says sometimes when you go back the second day, the bag breaks. But he still puts his laminaria in, and still waits for the next day. Well, once the bag breaks and you have a foreign body sitting there and the bacteria are getting from the vagina to the uterus, that’s a recipe for disaster.
…..
Q. You’re talking about the risk of infection?
A. Correct, and trauma to the cervix. If you are dilating the cervix to a greater degree, some of it is mechanical. You mechanically dilate first before he puts the first laminaria in. I have been told by some — the people, some or at least one of the people who does that, that they force as many laminaria in as possible on the second day because they want the greatest amount of dilatation as possible because that will make the delivery process easier. So it’s not just slow dilation from laminaria taking in fluid, there is some mechanical aspects to it too. And that, I think, does more risk to the cervix.
…..
Q. What kind of risk to the cervix are you talking to?
A. You traumatize the cervix. And there is information on earlier ones, which even dilate mechanically now, dilate the cervix either from 10 millimeters to 11 millimeters, it increases the risk of an incompetent cervix later. The cervix not being able to maintain a pregnancy or maybe just weak enough you have more preterm deliveries. And preterm deliveries are the single greatest medical obstetrical problem in the United States today.
…..
Q. Tell us what I’m done with that. Doctor, have you ever performed an intact D & X procedure?
A. I have not.
Q. In your practice, have you ever seen the need for it?
A. I have not.
Q. Your practice involves high risk obstetrics; is that correct?
A. Full range including high risk obstetrics and, again, I’m now president of a group of like 27, 28 OB providers. So I have seen a great number of circumstances. With our issues, they do clearly present them to me and I have never seen that.
Q. Would that be true even of situations involving serious maternal health conditions?
A. I have never seen a situation where a D & X would be the safest, the best, or the only procedure to use to protect the health of the mother.
Q. And that would be even in emergency situations where the pregnancy needs to be terminated and very quickly?
A. I have never seen a situation where intact D & X would be required, or the best procedure to do. In reading all the other declarations and stuff, I haven’t seen a single physician who provides it do that. The AMA committee that I sat on could — and there were several different obstetricians and Counsel on Scientific Affairs. Nobody could come up with a situation where the intact D & X would be necessary to preserve the health of the mother. In ACOG, when they had their panel, could not come up with — they couldn’t come up with a single example where it would be, you know, the best, most appropriate alternative to save the health of the mother or to have a beneficial effect on the health of the mother.
Excerpts from Government’s direct examination of Dr. Curtis Cook:
Q. When a pregnancy has to be ended prematurely, because of a maternal health condition of the kind that you treat, is it ever necessary to take a destructive act against the fetus directly, in order to protect the health interests of the mother?
A. No, all that is required for recovery of the mother is for separation of the fetus and placenta from her system so that she can start the recovery process. There is nothing inherent in the destruction of the fetus that starts to facilitate that process.
…..
Q. What is your response to the assertion that medical inductions are a more painful and physiologically stressful procedure than a surgical termination such as D&E?
A. Well, I think surgery is decidedly nonphysiologic as opposed to labor. So a labor induction is a much more physiological process or utilizes a natural process more than surgery would. But it also is a more controlled and monitored situation, as opposed to the D&X procedure, meaning that patients are constantly monitored for pain control, analgesia is constantly available to them in various forms, including patient controlled IV anesthesia or epidural, as opposed to having a handful of Motrin or Ibuprofen, going to a motel room somewhere for a couple of days while the cramping and contracting is taking place. [In a situation where labor is induced, a woman’s natural body process of expelling a baby is utilized instead of the unnatural D&E or D&X procedure. Also, in the case of inducing labor a woman’s condition is monitored more closely and pain managed in a superior way. More evidence that a partial birth abortion is not better for a woman’s health than giving birth.]
…..
Q. Doctor, the question was, in inductions, you have never used Digoxin or KCL to induce fetal demise in performing inductions, because you always considered it unnecessary; is that right?
A. That is not correct. I have not utilized those techniques but not because I consider them unnecessary ever. They haven’t been necessary for my clinical situations, because the people that utilize those techniques utilize it so they can guarantee that there is not a live born baby at time of delivery. And, if possible, I want a live born baby at time of delivery.
[Dr. Cook does not do abortions, but he does induce labor. The difference between an abortion and a live birth is simply not putting in medication to kill the unborn baby prior to causing labor. There is no medical risk involved in not doing this extra procedure]
DAY EIGHT: Thursday, April 8, 2004
Excerpts from Government’s direct examination of Dr. Elizabeth Shadigian:
Q. ….What is your opinion, with respect to assertions that the D&X procedure is intuitively safe, based on the experience of practitioners who are performing it?
A. Well, I know those practitioners have their best intellectual judgment in mind. And I know they want to be honest and truthful in what they are saying, but really it’s just anecdotal evidence they have that they think it’s safe. They don’t have any long-term studies or even a comparison of the D&X to another kind of procedure. So I don’t question that they really believe that, but really without data, we can believe a lot of things, but medicine is based on evidence. It’s based on doing studies. It’s based on comparison of what we know to what we don’t know. And in the absence of that, those are just anecdotal thoughts or feelings that a physician may have.
…..
Q. What’s your basis for that last assertion as to the follow-up of the abortion practitioners with their patients?
A. Well, there have been several studies. One, I quote specifically which is the Picker study from 1999, and they actually asked women about the quality of their abortion care, because this is such an important issue. And, in fact, it turns out that only about 29% of women actually follow up with their abortion provider afterwards. So it’s hard for me to understand how abortion providers, in quotes, know their complications, if they don’t even see their patients back later.
Share on Facebook

One thought on “PBA Trials: Nebraska”